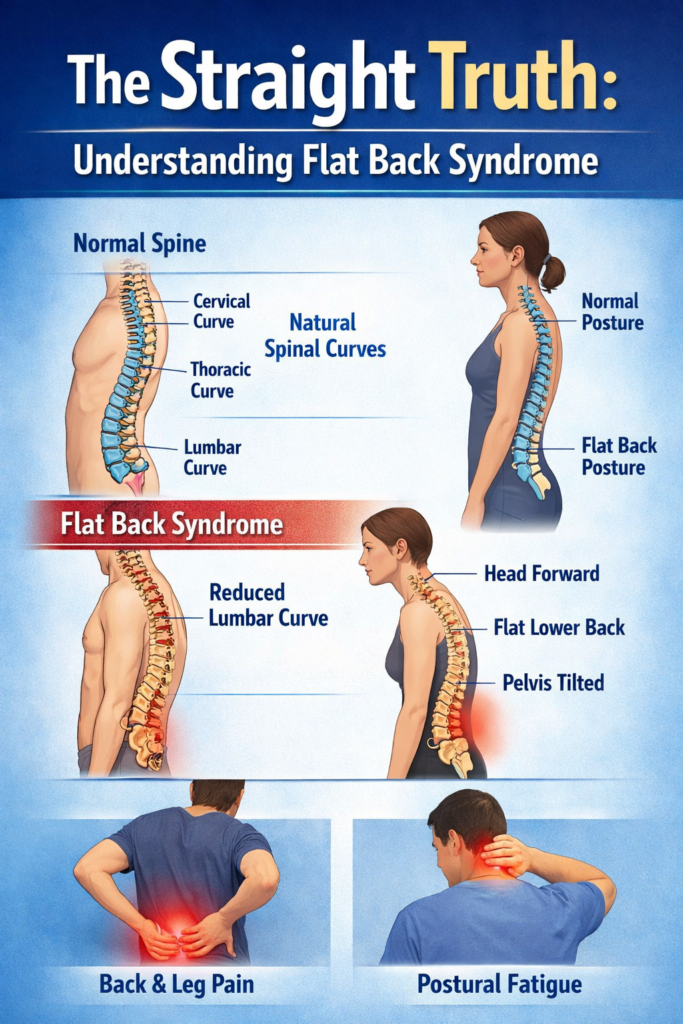
We often hear about the importance of “standing up straight,” but what happens when your spine becomes too straight? While a poker-straight back might sound like the pinnacle of good posture, the human spine actually relies on a series of elegant, natural curves to function correctly.
When those curves—specifically the inward curve of the lower back—disappear, it leads to a condition known as Flat Back Syndrome.
In this guide, we’ll explore the mechanics of the spine, why “flat” isn’t always “fine,” and how you can reclaim your natural alignment.
1. The Anatomy of a Healthy Spine
To understand Flat Back Syndrome, we first have to look at what a healthy spine looks like from the side. A normal spine is shaped like a gentle “S” curve. These curves act as natural shock absorbers, distributing the weight of your body and the stress of movement evenly.
There are two primary types of curves:
Kyphosis: The outward curves found in your mid-back (thoracic) and sacrum.
-
Lordosis: The inward curves found in your neck (cervical) and lower back (lumbar).
In Flat Back Syndrome, the lumbar lordosis flattens out. Without this inward curve, your center of gravity shifts forward, forcing your body to work overtime just to keep you standing upright.
2. What Causes the Spine to Flatten?
Flat Back Syndrome isn’t usually something people are born with; it is typically an acquired condition. Historically, it was a common side effect of early scoliosis surgeries (specifically those using “Harrington Rods” in the 1970s and 80s), but today, the causes are more varied:
Degenerative Disc Disease: As we age, the intervertebral discs that act as cushions between our vertebrae wear down. As these discs lose height, the spine can lose its natural curvature.
Compression Fractures: Often caused by osteoporosis, small fractures in the vertebrae can cause the spine to collapse forward.
Ankylosing Spondylitis: A chronic inflammatory arthritis that can cause the vertebrae to fuse together in a flattened or hunched position.
Post-Laminectomy Syndrome: Sometimes, surgery intended to relieve pressure on nerves can inadvertently lead to structural instability and a loss of lordosis.
3. The Symptoms: More Than Just a Flat Appearance
If you have Flat Back Syndrome, you won’t just notice it in the mirror. The symptoms are often progressive and can significantly impact your quality of life.
4. How It’s Diagnosed
If you suspect your spine is losing its curve, a specialist (usually an orthopedic surgeon or a physiatrist) will perform a series of tests.
Physical Exam: They will observe your gait and posture. A classic sign is a patient who needs to bend their hips and knees to maintain an upright gaze.
Full-Length X-rays: This is the gold standard. Doctors take a “standing lateral” X-ray from the side, covering the entire spine from the head to the pelvis.
The Plumb Line Test: Doctors use a virtual or physical weighted line dropped from the C7 vertebra (at the base of the neck). In a healthy spine, this line should pass through the sacrum. In Flat Back Syndrome, the line falls well in front of the pelvis.
5. Treatment Options: Reclaiming the Curve
The goal of treatment is simple: restore balance and reduce pain. Depending on the severity, there are two main paths:
Non-Surgical Management (The First Line of Defense)
For many, physical therapy is the primary solution.
Core Strengthening: Strengthening the abdominal and back muscles helps support the spine.
Hamstring Stretching: Tight hamstrings often pull the pelvis into a posterior tilt, worsening the flatness.
Bracing: In some cases, a specialized brace can help provide structural support
Surgical Intervention
If the imbalance is so severe that it prevents daily activities or causes neurological issues, surgery may be necessary. Modern procedures like an Osteotomy involve removing a small wedge of bone from the vertebrae to “re-bend” the spine into a more natural position.
6. Prevention and Daily Care
While you can’t always prevent degenerative changes, you can protect your “S-curve” with these habits:
Ergonomic Workspace: Ensure your computer monitor is at eye level so you aren’t constantly leaning forward.
Weight Management: Excess abdominal weight pulls the pelvis forward, putting extra strain on the lumbar region.
Movement Breaks: If you work a desk job, set a timer to stand and do gentle back extensions every 30 minutes.
