For anyone who has suffered from chronic back or neck pain, the promise of a “laser” solution sounds like something out of a science fiction utopia. Marketing campaigns for laser spine surgery often paint a picture of a bloodless, painless, “miracle” procedure that can have you back on your feet in hours.
However, in the medical community, the term “laser spine surgery” is often met with skepticism. While the technology is real, its application is frequently misunderstood—or intentionally overstated—by high-budget advertising. To make an informed decision about your spinal health, it is essential to look past the buzzwords and understand the actual science.
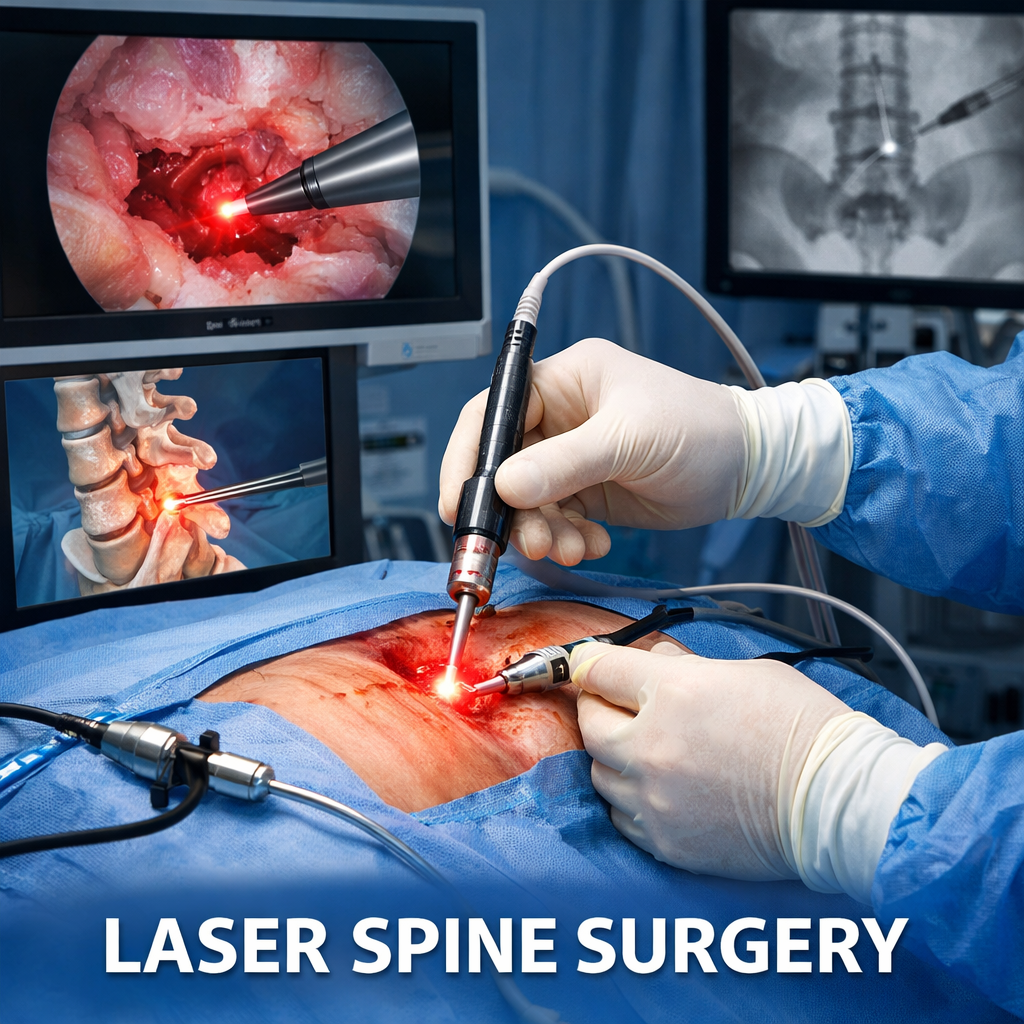
What is Laser Spine Surgery, Really?
In the strictest sense, laser spine surgery (LSS) is a procedure where a surgeon uses a focused beam of light to remove or shrink tissue.
It is important to understand that a laser is a tool, not a specialized surgical technique. In many “laser centers,” the laser is only used for a tiny fraction of the procedure—such as making the initial skin incision or debriding a small amount of soft tissue—while the actual heavy lifting is done with traditional surgical instruments.
The Two Common "Laser" Procedures:
Percutaneous Laser Disc Decompression (PLDD): A needle is inserted into a herniated disc, and laser energy is used to evaporate a small portion of the disc’s center, reducing internal pressure.
- Laser-Assisted Ablation: Used to remove small amounts of soft tissue or tumors that may be compressing a nerve.
The Marketing Hype vs. The Medical Reality
The gap between what you see on a TV commercial and what happens in a board-certified neurosurgeon’s operating room is significant. Let’s break down the common claims:
Claim 1: "It’s a Non-Invasive Miracle"
The Hype: Marketing often implies there are no incisions and no risks.
The Reality: All spine surgery requires an incision. While the cut may be small (under an inch), it is still an invasive procedure. Furthermore, the term “miracle” ignores the fact that LSS has a very limited range of use.
Claim 2: "It’s More Precise Than a Scalpel"
The Hype: A laser beam is presented as the ultimate tool for accuracy.
The Reality: In many ways, a laser is less precise than traditional instruments. A laser beam travels in a straight line and cannot “go around corners.” A surgeon using microscopic tools can navigate the complex, curved anatomy of the spine with far more nuance. Additionally, lasers lack the “tactile feedback” (the ability to feel the resistance of tissue) that surgeons rely on to avoid damaging nerves.
Claim 3: "It’s the Most Advanced Technology Available"
The Hype: It’s portrayed as the “Gold Standard” of modern medicine.
The Reality: Laser technology in spine surgery has been around since the 1970s. Most academic medical centers and top-tier neurosurgeons prefer Minimally Invasive Spine Surgery (MISS) or Endoscopic Spine Surgery. These techniques use high-definition cameras and micro-instruments that are widely considered safer and more effective than lasers for most conditions.
The Hidden Risks of Heat
One of the most significant medical “realities” omitted from marketing materials is thermal injury.
Because lasers work by generating intense heat to vaporize tissue, they can inadvertently damage surrounding structures. If a laser beam lingers too long near a nerve root, it can cause “heat spread,” leading to permanent nerve damage, increased pain, or even loss of function.
Scientific Fact: Unlike a scalpel, which cuts cleanly, a laser “boils” the water in cells. This can cause the surrounding tissue to experience inflammatory responses that are not present in cold-instrument surgeries.
When Does a Laser Actually Make Sense?
Is a laser ever the right choice? Yes, but in a very narrow set of circumstances. Medical literature suggests LSS may be appropriate for:
Small, contained herniated discs where only a minor reduction in pressure is needed.
Specific types of spinal tumors where a laser can help vaporize a mass without physical contact.
Debriding soft tissue in very specific, minor decompression cases.
It is almost never recommended for structural issues like spinal instability, scoliosis, or severe bone spurs, as a laser cannot cut through bone or stabilize vertebrae.
