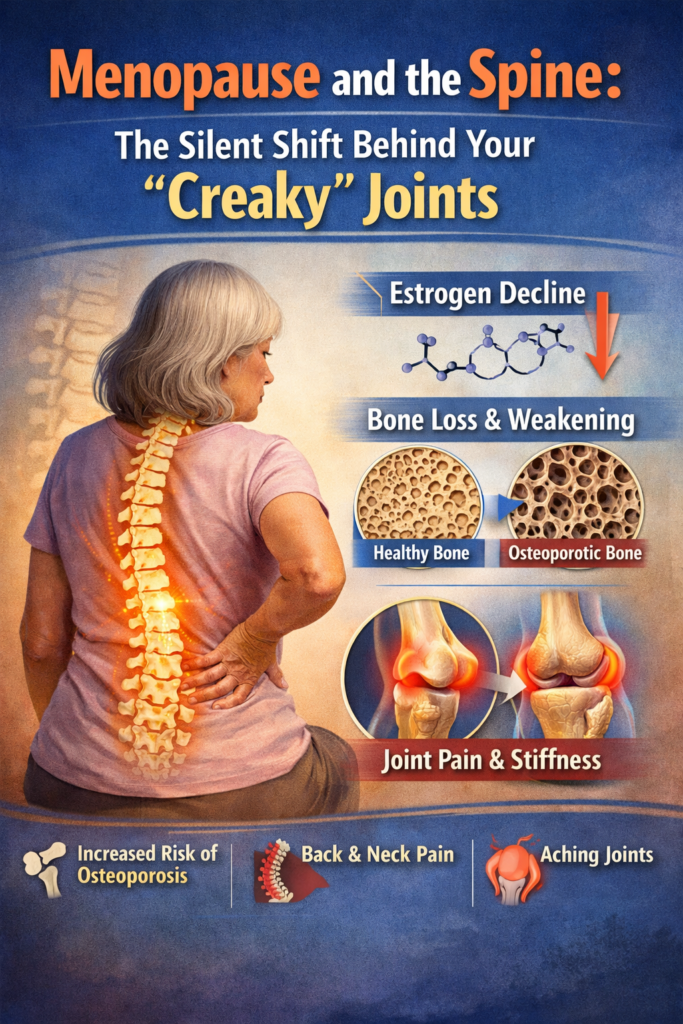
For many women, the transition into menopause is heralded by the usual suspects: hot flashes, night sweats, and mood swings. But there is another, more literal “growing pain” that often catches women off guard. One morning, you roll out of bed and notice your back feels stiffer than usual. Your neck cracks when you turn to check your blind spot while driving. Your knees emit a sound like dry autumn leaves being crushed.
It’s often dismissed as “just getting older,” but the reality is more biological than chronological. The sudden onset of “creaky” joints and spinal discomfort during menopause is deeply rooted in the dramatic hormonal shift—specifically the decline of estrogen.
In this deep dive, we’ll explore the intricate relationship between your hormones and your musculoskeletal system, why your spine is particularly vulnerable, and how you can navigate this “creaky” phase with strength and grace.
The Estrogen Connection: More Than Just Fertility
To understand why your spine feels like it needs a grease job, we have to look at estrogen’s “side hustle.” While we primarily associate estrogen with reproduction, it is actually a powerhouse hormone for the entire body. It acts as a natural anti-inflammatory and a vital regulator of bone and joint health.
1. The Natural Lubricant
Estrogen helps maintain the hydration of connective tissues. It keeps your cartilage—the rubbery tissue that cushions your joints—slick and resilient. When estrogen levels plummet during perimenopause and menopause, that “lubrication” decreases. This leads to increased friction in the joints, resulting in that hallmark “creakiness” and stiffness.
2. The Bone Protector
Estrogen is the primary guardian of bone density. It inhibits osteoclasts, which are the cells that break down bone. When estrogen disappears, bone resorption (breakdown) speeds up, while bone formation struggles to keep pace. This is why the risk for osteopenia and osteoporosis skyrockets during this window.
3. Inflammation Modulation
Estrogen is naturally anti-inflammatory. Its decline can lead to a systemic increase in pro-inflammatory cytokines. This is why many women experience “menopausal arthritis” or generalized joint pain (arthralgia) even if they’ve never had joint issues before.
Why the Spine Takes the Brunt
The human spine is a masterpiece of engineering, consisting of 33 vertebrae, dozens of joints (facet joints), and intervertebral discs. During menopause, this complex structure faces a “triple threat.”
The "Shrinking" Discs
Your spinal discs are the shock absorbers between your vertebrae. They are largely composed of water and collagen. Because estrogen plays a role in collagen production and water retention, the discs can begin to desicate (dry out) and lose height. This is one reason why some women find they are actually a half-inch shorter by the time they reach post-menopause.
As these discs thin, the space between vertebrae narrows, putting more pressure on the facet joints—the small joints that link your vertebrae together.
Facet Joint Osteoarthritis
When discs lose their “oomph,” the facet joints have to work harder. Without the protective buffering of estrogen-supported cartilage, these joints can become inflamed. This manifests as localized back or neck pain, particularly when you arch your back or twist.
The Muscle Support System
The spine doesn’t stand alone; it’s supported by a “corset” of core and back muscles. Estrogen decline is linked to sarcopenia, or the age-related loss of muscle mass and strength. When the supporting muscles weaken, the spine loses its external scaffolding, leading to poor posture and increased strain on the ligaments.
Recognizing the Symptoms: Is it Menopause or Something Else?
It can be difficult to distinguish between “normal” aging and menopause-related spinal changes. Look for these specific patterns:
Morning Stiffness: Feeling like a “tin man” for the first 30 minutes after waking up.
The “Creak” (Crepitus): Audible popping or grinding sounds in the neck or lower back during movement.
Loss of Flexibility: Difficulty reaching down to tie your shoes or looking over your shoulder.
Deep Aching: A dull, persistent ache in the lumbar (lower) spine that worsens after periods of inactivity.
Proactive Strategies: Silencing the Creaks
The good news? You aren’t powerless against your hormones. While you can’t stop the clock, you can change how your body responds to the shift.
1. Movement as Medicine
It sounds counterintuitive to move when you’re stiff, but movement is what “oils” the joints.
Weight-Bearing Exercise: Walking, hiking, or dancing helps maintain bone density.
Strength Training: Lifting weights is non-negotiable. Building the muscles around your spine (your erector spinae and abdominals) takes the physical load off your joints.
Yoga and Pilates: These focus on spinal decompression and core stability, which are vital for maintaining disc health.
2. Nutritional Foundations
Your spine needs specific raw materials to stay resilient:
Calcium and Vitamin D: The classic duo for bone health. Aim for $1200$ mg of calcium and at least $800$–$1000$ IU of Vitamin D3 daily (consult your doctor for personalized dosages).
Magnesium: Essential for muscle relaxation and bone matrix health.
Omega-3 Fatty Acids: Found in fish oil or flaxseeds, these help combat the systemic inflammation triggered by low estrogen.
3. Hydration
Since your spinal discs are mostly water, chronic dehydration can exacerbate “creaky” joints. Drink more water than you think you need, especially if you are also experiencing menopausal night sweats.
4. Hormone Replacement Therapy (HRT)
For many women, HRT can be a game-changer. By stabilizing estrogen levels, HRT can significantly reduce joint pain and slow the loss of bone density. If your spinal “creakiness” is severely impacting your quality of life, it’s worth a candid conversation with a menopause specialist to weigh the risks and benefits.
The Psychological Toll of the "Creak"
We often focus on the physical, but there is a psychological element to feeling “creaky.” It can make you feel “old” before your time, leading to a sedentary lifestyle out of fear of injury.
It is important to reframe this: Your body isn’t breaking; it’s recalibrating. By acknowledging that these changes are hormonal, you can strip away the “old age” stigma and treat it like the biological transition it is—much like puberty, but with better wisdom and (hopefully) better shoes.
