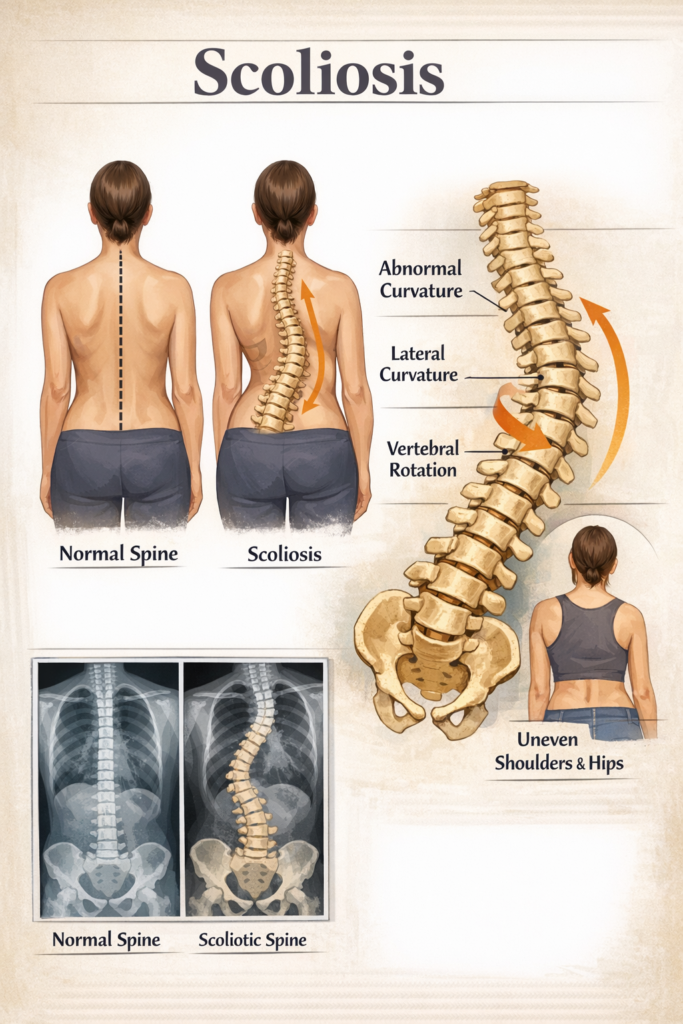
The image of scoliosis in the popular imagination is almost always a middle-schooler in a bulky plastic brace or a teenager undergoing a routine screening in a gym class. For a long time, the medical community treated scoliosis as a “pediatric problem”—something you either “fixed” before adulthood or lived with as a static condition once you stopped growing.
However, we now know that scoliosis doesn’t always stay in the past. For some, it’s a condition that first appears in their 50s or 60s. For others, a mild curve from youth begins to progress decades later. Adult scoliosis is a distinct clinical challenge, often intertwined with the natural aging process of the spine.
Understanding how to manage this curvature in later life is about more than just aesthetics or “straightening” the spine; it’s about preserving mobility, managing pain, and maintaining a high quality of life.
The Two Faces of Adult Scoliosis
To manage scoliosis in adulthood, we first have to identify which “type” we are dealing with. Medical professionals generally categorize adult cases into two groups:
1. Adult Adolescent Idiopathic Scoliosis (AdIS)
This is scoliosis that began during the teenage growth spurt but persists into adulthood. While many small curves remain stable, some can progress at a rate of roughly 0.5 to 2 per year. Over thirty or forty years, a “mild” 20-degree curve can become a 50-degree curve that causes noticeable physical changes and discomfort.
2. Adult De Novo (Degenerative) Scoliosis
This is a different beast entirely. “De novo” is Latin for “from the beginning.” This type of scoliosis starts in adulthood, usually after age 50. It is caused by the degeneration of the intervertebral discs and the facet joints. As these structural components wear down unevenly, the spine may begin to tilt or shift to one side, creating a “C” or “S” shaped curve where none existed before.
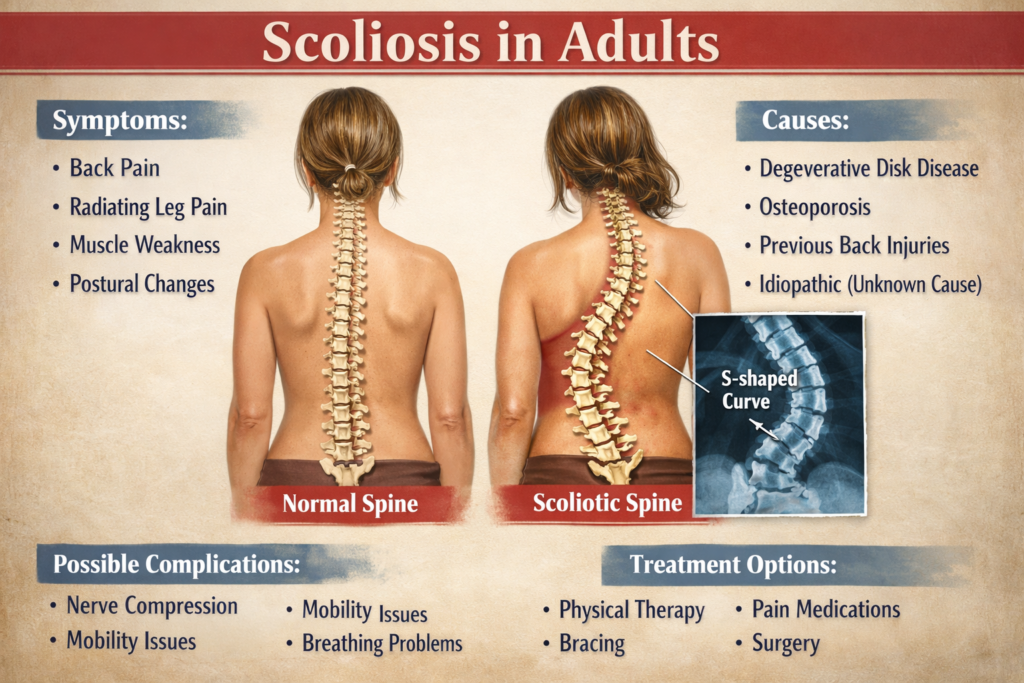
Why Does It Happen Later in Life?
The human spine is a masterpiece of engineering, but it is subject to the laws of physics and biology. Several factors contribute to why scoliosis becomes a concern in later life:
Disc Degeneration: Think of your spinal discs as shock absorbers. As we age, they lose water content and height. If a disc collapses more on one side than the other, it creates a “wedge” shape that forces the vertebrae above it to tilt.
Osteoporosis: Weakened bone density can lead to compression fractures. If a vertebra collapses asymmetrically, it creates a sudden bend in the spinal column.
Ligament Laxity: The ligaments that hold our vertebrae in alignment can become stretched or weakened, allowing for “micro-instability” that leads to curvature.
Muscle Imbalance: As core strength wanes, the muscles responsible for keeping us upright may fatigue unevenly, failing to provide the “internal bracing” the spine requires.
The Management Toolbox: Non-Surgical Approaches
The goal of treating adult scoliosis is rarely to achieve a perfectly straight spine. Instead, the focus is on functional restoration. Most adults can manage their symptoms effectively without ever stepping into an operating room.
Physical Therapy and "Schroth" Exercises
Generic “back exercises” are often insufficient for scoliosis. Specialized physical therapy, such as the Schroth Method, focuses on three-dimensional breathing and specific muscle engagement to help de-rotate and elongate the spine. It teaches the patient how to “find center” in their own body.
Core Strengthening and Low-Impact Conditioning
The spine depends on the “core” (the abdominals, obliques, and deep back muscles) for stability.
Pilates and Yoga: These are excellent for flexibility and core control, provided they are modified to avoid extreme spinal twisting.
Swimming: Taking the load of gravity off the spine while exercising is one of the best ways to build strength without triggering pain.
Pain Management and Injections
If nerve pain (sciatica) becomes debilitating, physicians may recommend:
Epidural Steroid Injections: To reduce inflammation around compressed nerves.
Facet Joint Blocks: To target pain arising from the small joints of the spine that are being stressed by the curve.
