If you’ve been experiencing persistent muscle weakness, unexplained tingling, or pain that feels like an electric shock, your doctor might have ordered an Electromyography (EMG). For most people, the name sounds like a complex Scrabble word, and the description—involving needles and electricity—can feel a bit daunting.
However, an EMG is one of the most effective tools modern medicine has for diagnosing neuromuscular disorders. Think of it as a specialized “listening device” for your body’s electrical grid. It allows doctors to hear and see how well your muscles and nerves are communicating.
In this guide, we’ll break down everything you need to know about the EMG: how it works, why you might need one, and what to expect when you’re on the exam table.
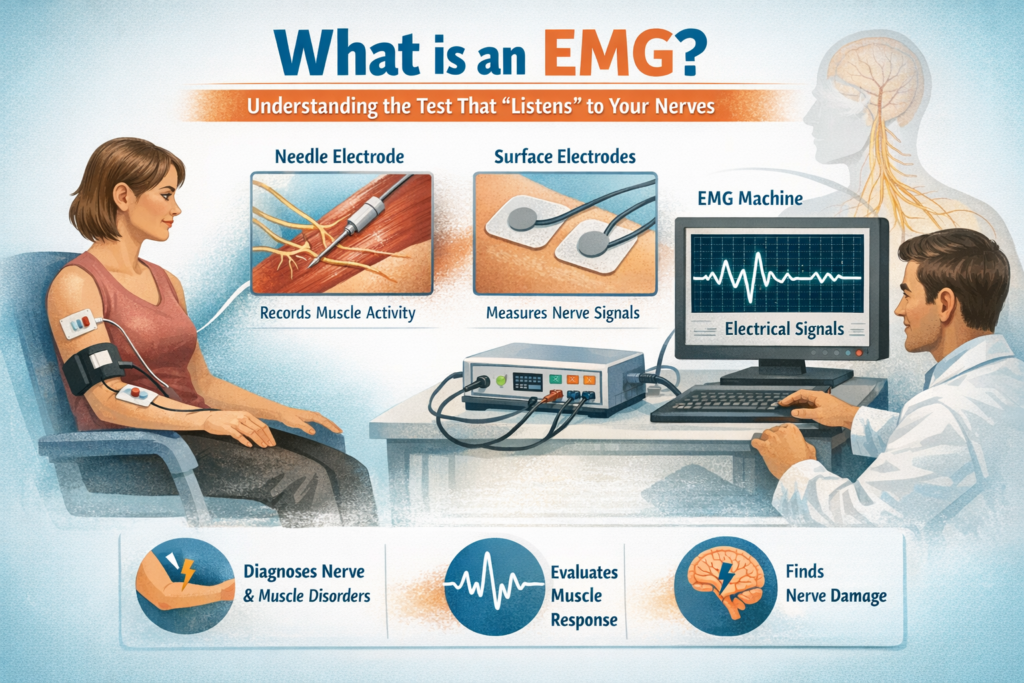
1. The Basics: What is an EMG?
At its core, an EMG is a diagnostic procedure that evaluates the health of muscles and the nerve cells (motor neurons) that control them.
Your body is essentially a bio-electric machine. Every time you decide to lift a finger or take a step, your brain sends an electrical signal down through your spinal cord and into your nerves. These nerves then “fire,” releasing a signal that tells your muscles to contract.
An EMG translates these electrical signals into graphs, sounds, or numerical data that a specialist (usually a neurologist or physiatrist) can interpret.
The Two Components of the Test
Most “EMG tests” actually consist of two distinct parts performed during the same appointment:
Nerve Conduction Study (NCS): This part uses electrodes taped to the skin to measure how fast and how strongly electrical signals travel through your nerves.
Needle EMG: This part involves inserting a very thin needle electrode into specific muscles to record the electrical activity within the muscle fibers themselves.
2. Why Would You Need an EMG?
Doctors don’t usually order an EMG as a first-line “just because” test. It is typically used to investigate symptoms that suggest a problem with the “wiring” of the body. You might be referred for an EMG if you experience:
Numbness or Tingling: Often described as a “pins and needles” sensation.
Muscle Weakness: Difficulty lifting objects or walking that doesn’t improve with rest.
Chronic Pain: Specifically radiating pain (like sciatica) or burning sensations.
Cramping or Twitching: Involuntary muscle movements (fasciculations).
Common Conditions Diagnosed
An EMG is vital for identifying several different types of issues:
Carpal Tunnel Syndrome: Pressure on the median nerve in the wrist.
Herniated Discs: Pinched nerves in the spine (radiculopathy).
Neuropathy: Nerve damage often caused by diabetes or toxins.
Muscular Dystrophy: Disorders that affect the muscle fibers themselves.
ALS (Lou Gehrig’s Disease): Conditions that affect the motor neurons in the brain and spinal cord.
4. Preparing for the Test: What You Need to Know
The good news? There isn’t much “homework” for an EMG. However, following these steps ensures the test is accurate and as comfortable as possible:
Skip the Lotion: On the day of the test, do not apply oils, lotions, or creams to your skin. These can interfere with the electrodes’ ability to pick up electrical signals.
Temperature Matters: If your hands or feet are very cold, it can slow down nerve conduction and lead to inaccurate results. Most clinics will have you sit in a warm room or use heating pads before starting.
Medication Check: Most medications are fine, but if you are taking blood thinners (like Warfarin) or have a pacemaker, you must tell your doctor beforehand.
Dress Comfortably: Wear loose-fitting clothes. You may be asked to change into a hospital gown depending on which area is being tested.
4. Step-by-Step: The EMG Experience
Part 1: The Nerve Conduction Study (NCS)
The doctor or technician will start by cleaning your skin. They will then tape several “recording electrodes” to your skin over the nerve being tested.
Next, they will use a handheld stimulator to deliver a small, brief electrical pulse to the nerve. It feels like a static electricity shock or a rubber band snapping against the skin. While it can be startling, it is not generally described as painful. The computer records how long it takes for your muscle to react to that shock.
Part 2: The Needle EMG
This is the part that makes people nervous, but it’s actually the most “listening-focused” part of the test.
The doctor inserts a fine, thin needle (about the size of an acupuncture needle) into the muscle. There is no “injection”—the needle acts as a microphone.
Resting Phase: The doctor will ask you to relax. A healthy muscle should be electrically “silent” at rest.
Contraction Phase: You will be asked to flex the muscle slowly. As you do, the monitor will show spikes and waves, and you will hear a sound through a speaker that sounds like hail on a tin roof or radio static.
5. Does it Hurt? (The Candid Truth)
Let’s be real: having needles stuck in you and being shocked isn’t exactly a spa day. Most patients describe the sensation as uncomfortable rather than unbearable.
The “shocks” during the NCS are very brief. During the needle portion, you may feel a sharp prick as the needle enters, and a dull ache while it’s in the muscle. The key is to stay as relaxed as possible; tensing up can actually make the test take longer and feel more intense.
Post-test: You might feel some minor muscle soreness or see small bruises at the needle sites for a day or two. There are no lasting side effects.
