For decades, the standard of care for chronic back and neck pain—when conservative treatments failed—was clear-cut: “fuse it.” If a disc was damaged, surgeons would remove it and weld the surrounding vertebrae together to stop the painful motion.
However, as we move through 2026, a paradigm shift is occurring. Patients are no longer just asking to be “pain-free”; they are asking for mobility. This shift has placed Artificial Disc Replacement (ADR) and Spinal Fusion at the center of a high-stakes debate: which procedure truly represents the future of spine care?
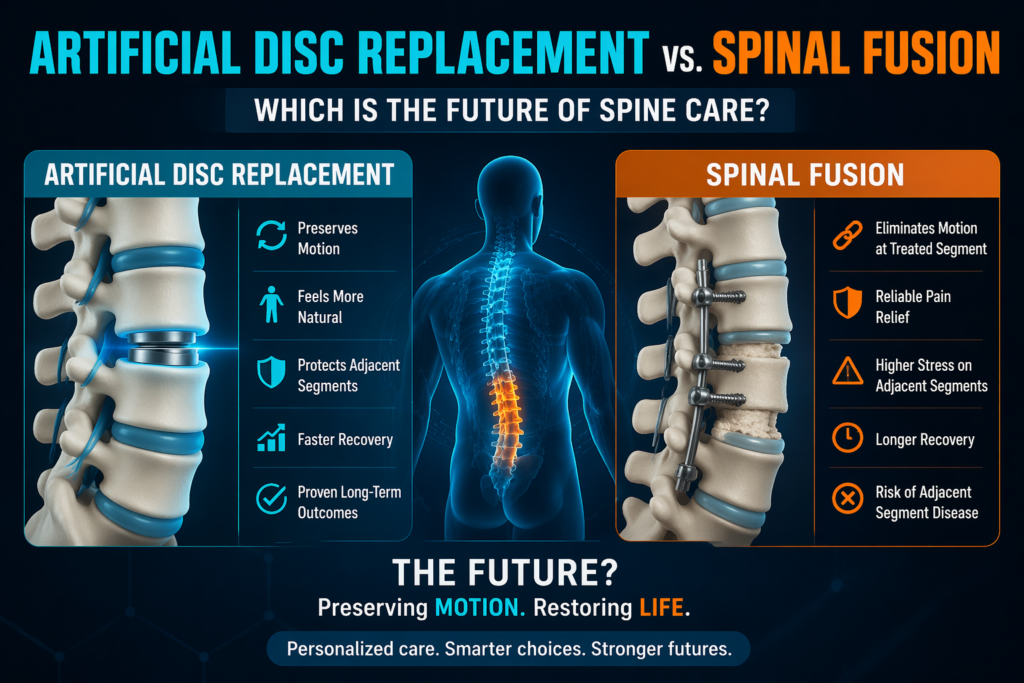
The Contenders: Understanding the Tech
To understand where the field is going, we must first look at how these two procedures fundamentally differ in their approach to spinal mechanics.
1. Spinal Fusion: The "Gold Standard"
Spinal fusion (such as ACDF in the neck or TLIF in the lower back) is designed to create stability. The surgeon removes the problematic disc and uses bone grafts, cages, and screws to encourage the two vertebrae to grow into a single, solid bone.
The Goal: Eliminate motion to eliminate pain.
The Reality: It is incredibly effective at stopping pain caused by instability, but it permanently alters how the spine moves.
2. Artificial Disc Replacement (ADR): The "New Frontier"
Also known as disc arthroplasty, ADR takes the opposite approach. Instead of locking the joint, the surgeon replaces the damaged disc with a mechanical device made of medical-grade metal and high-density plastic.
The Goal: Mimic the natural movement of a healthy human disc.
The Reality: It seeks to preserve flexibility and reduce the stress placed on the “neighboring” levels of the spine.
Comparing the Outcomes: The 2026 Data
In the past, fusion was the default because we lacked long-term data on how artificial discs held up over time. In 2026, the data is in, and it’s revealing some striking trends.
Mobility and Range of Motion
The most obvious advantage of ADR is the preservation of motion. Clinical studies now show that patients who undergo ADR maintain significantly more “natural” movement patterns. This is particularly vital for younger, active individuals who want to return to sports or physically demanding jobs. Fusion, by design, creates a “stiff” segment, which can sometimes lead to a feeling of limited flexibility.
The "Adjacent Segment" Problem
The Achilles’ heel of spinal fusion has always been Adjacent Segment Disease (ASD). When you fuse one level of the spine, the levels above and below it must work harder to compensate for the lost motion. This extra “mileage” causes those healthy discs to wear out faster, often leading to a second surgery years later.
Recent meta-analyses (2025–2026) suggest that ADR may reduce the risk of ASD. By allowing the treated level to continue moving, the mechanical stress is distributed more naturally, potentially protecting the rest of the spine.
Recovery Speed
Because ADR does not require the body to grow new bone (a process that can take 6 to 12 months), the initial recovery is often faster.
Fusion Recovery: Often involves 3–6 months of restricted activity and bracing.
ADR Recovery: Many patients are cleared for light activity within 6 weeks and full activity within 3 months.
| Feature | Spinal Fusion | Artificial Disc Replacement |
| Primary Mechanism | Stabilization (No motion) | Motion Preservation |
| Recovery Time | 6–12 Months | 3–6 Months |
| Long-term Risk | Adjacent Segment Disease | Implant wear or loosening |
| Track Record | 50+ Years | 20+ Years |
| Candidacy | Broad (Arthritis, Deformity) | Selective (Healthy joints) |
Recent meta-analyses (2025–2026) suggest that ADR may reduce the risk of ASD. By allowing the treated level to continue moving, the mechanical stress is distributed more naturally, potentially protecting the rest of the spine.
Why Isn't Everyone Getting an Artificial Disc?
If ADR preserves motion and speeds up recovery, why isn’t fusion obsolete? The answer lies in patient selection.
ADR is a high-performance solution for a very specific problem. To be a candidate for an artificial disc in 2026, you generally need:
Good Bone Quality: Osteoporosis can cause the metal implant to “sink” into the bone.
Healthy Facet Joints: If the small joints in the back of your spine are already arthritic, an artificial disc won’t help; in fact, moving an arthritic joint will only cause more pain.
Minimal Deformity: ADR cannot correct significant scoliosis or spinal “slippage” (spondylolisthesis) as effectively as fusion.
Spinal Fusion remains the “hero” for complex cases. For patients with severe instability, multi-level degeneration, or significant deformity, fusion provides a level of structural correction that an artificial disc simply cannot match.
The Hybrid Approach: A Middle Ground
The future may not be an “either/or” scenario. We are seeing a rise in Hybrid Surgery. In these cases, a surgeon might fuse a severely unstable level while placing an artificial disc at the level above it. This “best of both worlds” strategy provides the necessary stability while trying to mitigate the risk of adjacent segment wear.
The Verdict: Which is the Future?
In 2026, we are moving toward Personalized Spine Care.
The “Future of Spine Care” isn’t a single device; it is the sophisticated selection of the right tool for the right patient. * Artificial Disc Replacement is the future for the active, middle-aged patient with localized disc disease who wants to maintain a high level of physical performance.
Spinal Fusion is the future for complex reconstructions, deformity correction, and the aging population with significant bone and joint wear.
